Healthcare providers (HCPs) and healthcare professionals (HCProfs) are welcome to join the Electronic Health System (eHealth) and view their patients' electronic health records (eHRs) in eHealth even they do not use any electronic medical record (eMR) system and have no health record to be shared to eHealth yet.
However, it is still advisable for HCPs and HCProfs to explore implementation or upgrade of their record systems for sharing.
View eHRs
eHealth is designed to provide an additional platform for sharing information of patients among HCPs and HCProfs.
According to the Code of Practice, HCProfs shall exercise professional judgement to interpret the information on eHealth and to consider how much information shall be accessed for reference purposes. Such judgement should be exercised on a case-by-case approach and based on the need for providing care to individual patient.
Share eHRs
Data within the sharable scope for sharing can be shared to eHealth. To promote transparency and respect patients' rights, the data categories that can be uploaded by HCP's eMR system will be published at the HCP Register.

Software available for uploading eHRs
The eHR Office has developed the following free Clinical Management Systems (CMS) for private sectors to facilitate computerisation of their record systems and make health information of their patients sharable on eHealth.
There are also software solutions available in the market for use by HCP. The eHR Office works with major vendors of clinic software to enhance their products to support data sharing with eHealth.

Uploading eHRs timely
In general, HCPs shall upload the health data in their medical record systems to eHealth for sharing as soon as possible and reasonable after each episode of care.
The timeliness to process the data before it is shared to eHealth may be justified with various clinical reasons (e.g. quality check, authorisation of certain reports and processes required in completing the patients' records etc.) and technical reasons (e.g. data consolidation, retrieval, checking and packaging etc.).
Individual HCPs may approach the eHR Registration Office (hotline no.: (852) 3467 6230) to discuss and agree on the arrangement for data uploading.
Documentation at eHealth
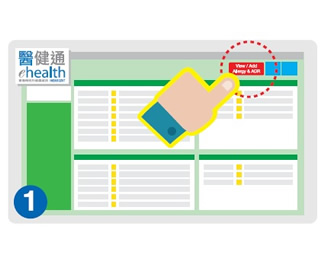
Inputting Allergy and Adverse Drug Reaction (ADR) Records
The Allergy and Adverse Drug Reaction (ADR) input module can be accessed via the eHR Viewer by medical practitioners, registered or enrolled nurses and registered dentists of eHealth HCPs. The function aims to enhance medication safety by encouraging HCPs' sharing of patients' allergy and ADR records via eHealth.
Who can access?
All HCPs are given access to the Allergy and ADR input module except those that are already uploading allergy and ADR records to eHealth or those that are technically ready to do so. Access to the module will be granted to eligible HCPs by default. Prior enrollment or set up is not required.
HCProfs who have joined the Public-Private Partnership (PPP) programmes of the Department of Health and the Hospital Authority can also access the module via the respective PPP applications.
Core features
The module provides the following user-friendly features –

1. Built-in smart search of allergen and ADR causative agent

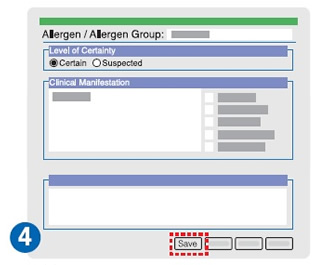
2. Efficient documentation via selection panel

3. Update and deletion of a particular data entry in the record
The new record will then be shown on the eHR Viewer immediately for sharing.
A quick guide and a detailed user guide on the above function are now available at the eHealth portal for HCProfs' easy reference (User Documents - User Guide for Allergy and ADR Input Module).
Related information
Frequently asked questions
-
Can I access a patient's eHR whom I do not have sharing consent but is unconscious and in emergency?Expand
- You may request for Emergency Access to the patient's eHR only if the patient is unable to give sharing consent (e.g. unconscious) and also under the following circumstances in which the lack of access to the patient's eHR would likely:
- cause serious harm to the physical or mental health of the patient;
- cause serious harm to the physical or mental health of any other individual; or
- prejudice the carrying out of emergency rescue operations or provision of emergency relief services.
- All access and use of eHR (including Emergency Access) in eHealth must be under proper authorisation and will be logged and subject to audit.
- You may request for Emergency Access to the patient's eHR only if the patient is unable to give sharing consent (e.g. unconscious) and also under the following circumstances in which the lack of access to the patient's eHR would likely:
-
Can I use patient's information for pre-attendance care or post discharge follow up when patient is not physically with me?Expand
- Before patient actually receives care e.g. before attendance or pre-admission, access to the patient's eHR is acceptable but shall be cautious. It is advisable to inform the patient in advance (e.g. upon appointment booking) about such possible access.
- After patient having received care and having been discharged, it is acceptable to access the patient's eHR if it is indicated. It is also advisable to inform the patient in advance the possible access.
- HCProf should be aware that the patient will receive notification for access to his / her eHR.
-
Can I print out or directly capture the information from eHealth to my own clinical record?Expand
- You should clearly indicate the source of information, date / time of the information being accessed when copying information from eHealth to your own clinical records.
- You should be aware that information printed out may be outdated and not comprehensive.
- According to the Code of Practice (COP) (Section 2.5), you should ensure proper filing and record keeping of any printed health records of patients from eHealth. You should also act in accordance with the record management policies of your healthcare organisation.
-
I am worried that my patients may request me to access their eHRs and challenge the services provided by other HCProfs. How can I respond to them?Expand
- You should explain to the patients that the purpose of eHealth is for supporting direct patient care but not to retrieve information to challenge or comment the services provided by other HCProfs.
- According to the COP (Section 3.4) and the Professional Conduct and medical ethics,
- It is inappropriate to use the information obtained from eHealth to allege challenges or criticism in whatever means to disparage or depreciate the professional skills, knowledge, services or qualification of other HCProfs and / or HCPs.
- HCProfs, however, are not prohibited from making fair and honest comments on another HCProf if the professional conduct or competence of him / her may be called into question.
-
How can I view patient’s radiology images?Expand
To view patient’s radiology images, you can simply click the radiology image record’s icon. The image(s) will be displayed in a pop-up Image Viewer.
In general, you can view last 2 years of patient’s radiology images that uploaded by the HCPs.